Your HUB's Biggest Problem Was Never the Technology
Using AI to Enhance Patient Experience in HUB Services
Ankur Jain, Esq. (J.D., MBA, POPM, SAFe Agilist)
3/4/20264 min read


Since 2015, I have worked on platform for HUB services connecting patients, payers, providers and pharmacies
At the center of the diagram — where the intelligent routing engine should go — I wrote three letters in a box:
T — B — D.
To Be Determined.
Not because we didn't know what was needed. We did. The HUB was processing thousands of patient referrals a year. 90% of incoming calls had pre-defined answers sitting in an ops wiki nobody could get to fast enough. Enrollment was still running on faxes — 15 to 20 minutes of manual data entry per patient, per referral. I knew what AI should be doing here. I just couldn't build it yet.
That TBD box has been filled in.
And what's replaced it isn't just better software. It's a different architecture entirely.
The legacy HUB model was an architectural accident — benefits investigation from one vendor, prior authorization from another, patient enrollment from a third, CRM layered on top. Each system optimized for its own KPIs. Nobody owned the full patient journey.
What's emerging now is vertically integrated: one platform owning the clinical decision layer, the hub automation layer, the prescription routing layer, and the patient touchpoint — as a single native system. That's not an upgrade. That's a rebuild.
The market data reflects exactly that shift:
📊 The pharma HUB and patient access support market hit $3.24 billion in 2024. It's projected to reach $7.63 billion by 2033 — growing at 10% annually. AI is the primary growth driver.
🔗 Starting January 1, 2027, U.S. payers must deploy three FHIR APIs — Coverage Requirements Discovery, Documentation Templates & Rules, and Prior Authorization Support — that create the real-time, interoperable data layer HUBs have needed for years. The infrastructure bottleneck I mapped in 2018 is being legislated away.
⚡ EVERSANA's ACTICS eAccess platform connected to 1,400+ payers and completed 92% of benefits verifications in real time — under one minute — with initial PA acceptance rates improving 25%. What once took days now takes seconds.
🤖 Wellgistics Health launched HubRx AI in late 2025 — a full-stack agentic AI engine integrating with leading LLMs (ChatGPT, Claude, Gemini) to automate eligibility checks, prior authorization, claims management, and patient adherence workflows end to end.
Research by HIMSS Analytics shows AI-driven PA automation delivers a 60% reduction in processing time and 35% decrease in administrative costs. Industry data shows agentic AI models can handle 60%+ of scheduling and status-check calls autonomously — with roughly 50% call cost reduction.
But the most important shift isn't in any single metric. It's in what these platforms are doing architecturally.
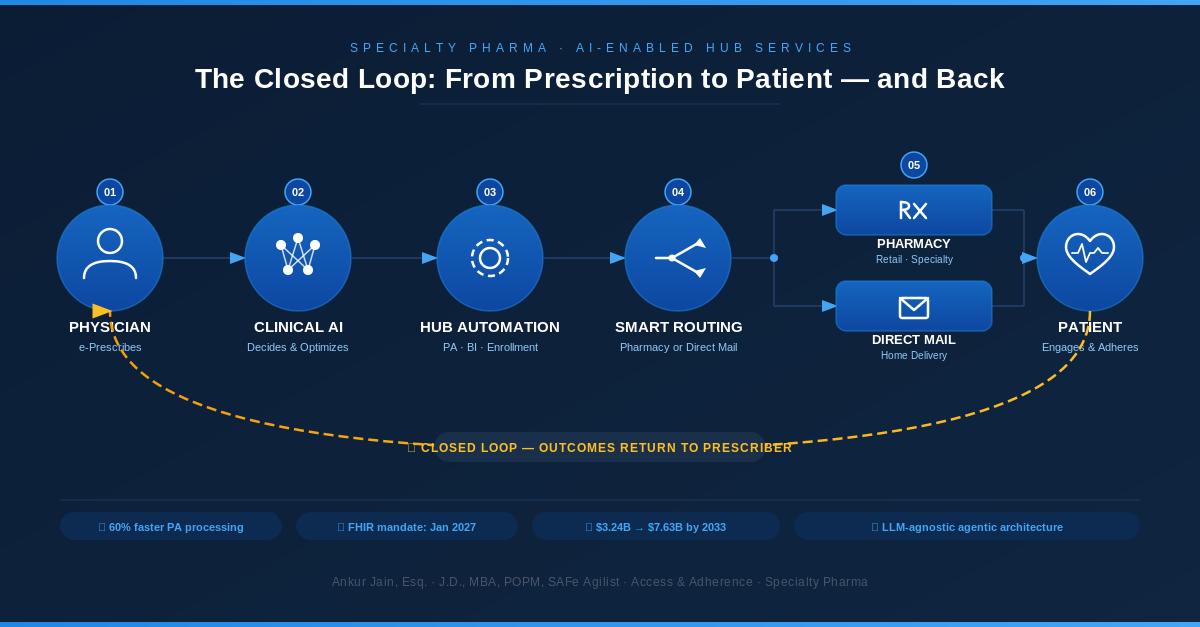
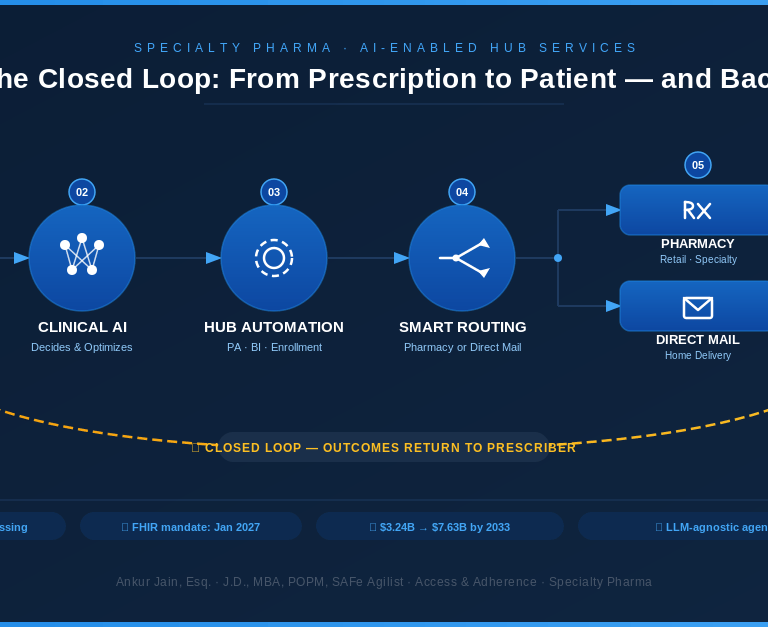
They're closing the loop.
In the old model, each step was a silo — verify benefits, process PA, enroll the patient, hope someone calls the pharmacy. Data moved in one direction: forward, and often lost. The new architecture reverses that. Adherence data feeds back to the prescribing physician. Fulfillment confirms to the manufacturer. Payer outcomes fold back into clinical decision logic. The AI isn't just processing transactions faster — it's learning from every one and routing that intelligence upstream to every stakeholder in the chain.
That's a fundamentally different system than what I was mapping in 2018.
So the TBD problem is solved. But a new challenge has taken its place.
Here's what I'm watching closely in 2026:
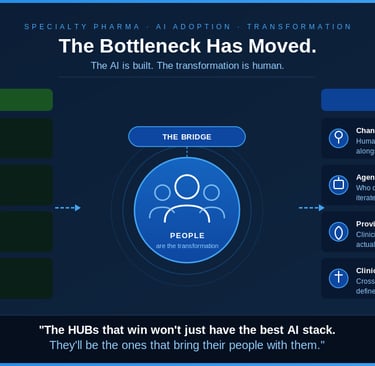
The bottleneck has shifted from technology to transformation.
The agentic AI is ready. The FHIR interoperability layer is coming by mandate. The platforms exist. But in most HUB operations I've studied, the systems, teams, providers, and patients aren't ready to absorb this change at the speed the technology can deliver it.
And there's a capability gap hiding inside the excitement.
The technology now lets you design, deploy, and manage specialized agents — one for eligibility verification, one for prior authorization, one for adherence outreach, one for copay card application. Each trained. Each monitored. Each improvable over time.
BIGGEST PROBLEM TO ADOPTION:
But who in your organization is going to own that?
It's not a pure IT function. It's not a pure operations function. It requires clinical knowledge to define the agent logic, operational expertise to map the workflow, and change management discipline to keep agents aligned as your programs evolve. Most HUBs don't have that team yet — and most vendors aren't building it for you.
I've seen this before. In 2022, we rebuilt a patient enrollment portal — fully modern, omni-channel, beautifully designed. Patient adoption went from 3% to 60%. But not because the technology was perfect on day one. Because we invested as much in the human transition as we did in the technical build.
The HUBs that will win in 2026 won't just be the ones with the best AI stack.
They'll be the ones that can get their agents, providers, and patients to actually trust it, use it, and integrate it into how they work — quickly, sustainably, and without burning out the people who keep the HUB running today.
That's the transformation gap I built Artha Consulting to close.
We don't just implement AI. We design the human journey alongside it — so that the technology actually takes hold and delivers the patient outcomes the industry is capable of.
The TBD is no longer the AI. The TBD is whether your organization is ready for it.
💬 I'd love to hear from people working inside HUB operations or specialty access programs: What's the biggest barrier you're seeing to AI adoption right now — the technology, the people, or the process?
#SpecialtyPharma #HUBServices #PatientExperience #HealthcareAI #AccessAndAdherence #AgenticAI #DigitalTransformation #FHIR #PatientSupportPrograms #ArthaConsulting #ChangeManagement #LifeSciences